The first knee arthroscopy (1918) is attributed to Takag (Japan). However, the arthroscope will remain for a long time an object of research and diagnosis, until Mr. Watanabe (Japan) publishes in 1957 the first edition of his Atlas and invents the arthroscope n° 21, allowing a more complete observation. articulation and taking color photos. The publications that appeared helped spread the method. The progress made in equipment and the creation of learned societies have made it possible to make progress and codify techniques. The appearance of miniaturized equipment to which Terry Whipple largely contributed later made possible the development of arthroscopy of the wrist and the joints of the hand.
Arthroscopy has played a role (and still plays a role) in the deeper understanding of joint physiology and how to approach pathologies, in close correlation with clinical and imaging.
Principles of the intervention
Patients are generally operated on as outpatient surgery, under locoregional anesthesia. The use of appropriate equipment for each intervention is necessary. However, there is common equipment for all arthroscopies which consists of a color flat screen, an adapted camera, a cold light source, an arthrpomp, an arthroscope, a shirt and introducer, a feeler, cutting and non-cutting pliers, a shaver (motorized abrasive material for soft parts) and a motorized cutter for the bone.
This surgery is generally performed in the supine position on an ordinary table. The practitioner performs a tourniquet at the root of the limb, limb fixed or towed according to the habits of the operator and the joint in question. Antibiotic prophylaxis is necessary.
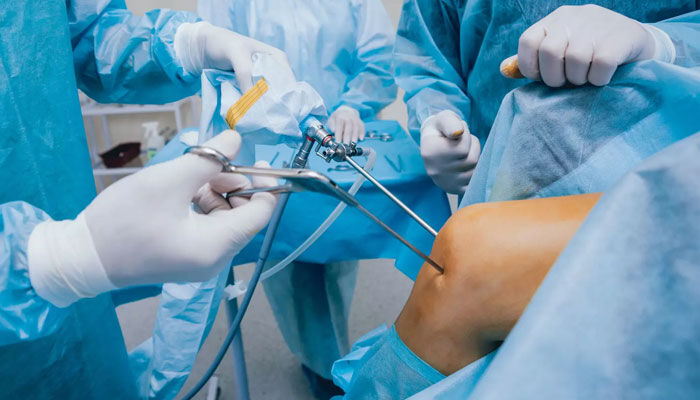
The approaches are generally two or three in number, and allow the introduction of optics and instruments. The practitioner proceeds to the articular filling with saline solution under pressure and sets up the shirt with introducer. It introduces the optic whose size varies according to the joint: 4 mm for the knee, the hip, the ankle and the shoulder, and 2.7 mm for the wrist and the elbow. A lesional assessment is first established, facilitated after careful debridement with a shaver, especially in the event of interposition of the soft tissues in front of the camera. The therapeutic gesture can begin with or without immobilization of the limb (according to the request of the technique).
The postoperative follow-up is generally simple and the functional and aesthetic results are excellent, allowing the early resumption of professional and sports activities.
However, even though arthroscopy has the reputation of being a benign procedure, statistics show some complications. Even if they are rare, they are a constant concern for the medical team and this risk explains why certain additional examinations or treatments are prescribed.
Multiple Indications
There are many indications for arthroscopy. Meniscal and ligament lesions account for more than half of operations. Synovial pathology, cysts, bone necrosis, joint fractures, osteoarthritis are also lesions that can possibly be treated with this technique.
A meniscal lesion is a classic indication for knee arthroscopy. When a meniscus is damaged, it becomes bothersome and arthrogenic and the patient suffers from joint blockages. It is possible to remove the phatological meniscus. The principle of this intervention is to resect only the injured part of the meniscus, keeping its part intact, so as to spare its role as a shock absorber as much as possible. In some cases, if the lesion is in the peripheral area, a meniscal suture is indicated.
Intrinsic ligament lesions have a significant impact on the biomechanism of the joint and can cause functional sequelae and joint degeneration (osteoarthritis). Non-invasive repair has become possible using arthroscopy. In practice, lesions of the anterior and posterior cruciate knees require ligamentoplasty, sometimes urgently in young athletes.
Synovial popliteal cyst is usually caused by meniscal degeneration. Arthroscopy will be the method of choice to solve this problem. It is necessary to regularize this degenerative meniscal lesion and not to remove the cyst. The cyst (the consequence) will only disappear once the intra-articular lesion (the cause) has been treated.
Arthroscopy also plays a role in the treatment of joint fractures, the anatomical reduction of which prevents the occurrence of post-traumatic osteoarthritis. The intervention begins with evacuation of the hemarthrosis and washing. An exploration looks for a possible ligament or meniscal lesion. Once the lavage and the joint assessment have been carried out, the fracture is reduced using a spatula. The practitioner performs osteosynthesis of the fracture under arthroscopic and image intensifier control.
Septic and aseptic synovial lesions are quite frequent pathologies (osteochondromatosis, villonodular synovitis, synovial hemangioma, Hoffa's disease.
Synovial osteochondromatosis is a metaplasia of synovial tissue such that it produces small rounded cartilaginous bodies that protrude from the inner surface of the synovium, pediculate and then detach becoming loose foreign bodies in the joint cavity. The intervention under arthroscopy confirms the diagnosis and eliminates the majority of foreign bodies.
Villonodular synovitis is a tumoral degeneration of the synovium. This tumor appears as a well-circumscribed, lobulated mass, adherent to the capsule or ligament, firm or hard, varying in color from yellowish-white to rusty brown. These tumors measure from a few millimeters to 3 or 4 centimeters in diameter.
The disease described by Hoffa is characterized by a significant hyperplasia of the adipose ligament of the knee which develops behind the patellar ligament, under the tip of the patella. The knee can also be the seat of an arborescent lipoma which represents a particular hyperplasia of the synovium whose multiple fringes, often very long, are made up almost exclusively of adipose tissue. A simple resection of it solves the problem.
Technique to be developed
The importance of arthroscopy no longer needs to be demonstrated because it offers the advantage, compared to conventional surgery, of being non-traumatic and aesthetic while being just as effective. However, it should not be forgotten that this is an expensive technique that uses fragile equipment and requires a long and particularly supervised learning process. However, it deserves to be developed and encouraged.
