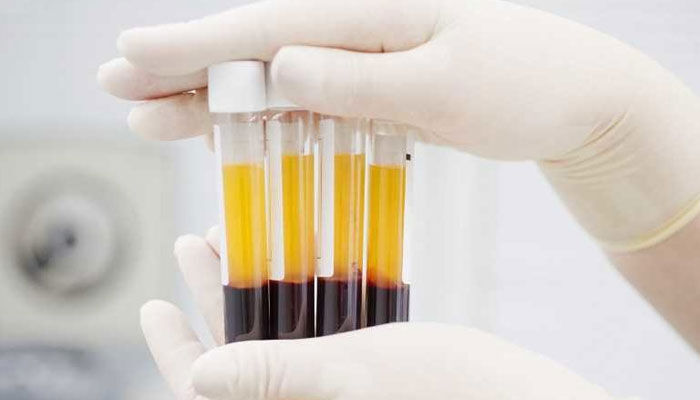
PRP, Platelet Rich Plasma
PRP is a concentrate of platelets about 5 times higher than the normal rate, obtained by centrifugation of autologous blood, taken from the patient, about 60cc, which allows the removal of other blood compounds, red and white blood cells. It is also obtained, but in a smaller volume, after centrifugation of bone marrow. PRP has healing properties through its growth factors.
- These platelets (responsible for the formation of clots during blood coagulation) release, in contact with the osteocartilaginous lesion of the knee, or ligament and tendon lesions, a dozen powerful proteins contained in the alpha granules of the platelets, released during activation of platelets, and responsible for tissue healing.
PRP can accelerate the healing process of knee osteoarthritis: cartilage and meniscal damage; ligament or tendons, alone or associated with stem cells, due to the presence of essential growth factors including: platelet-derived growth factor (PDGF), transforming growth factor beta (TGF beta), etc. stimulating the formation of vessels, bone cells, cartilage, etc.
PRP is in liquid form, It can be transformed into gel form: Platelet Gel, in 5 seconds, by mixing it with a mixture of thrombin and calcium chloride, allowing the powerful healing components to remain in place during application. The Gel platelet is useful in certain clinical cases.
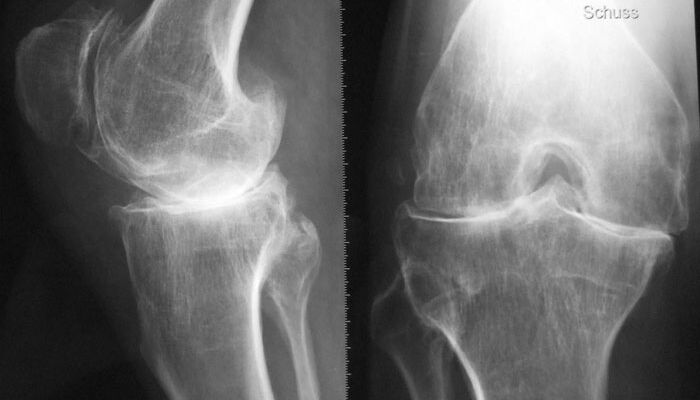
PRP injection:
- It is done under local anesthesia or light sedation.
- Aseptic preparation of the injection area.
- Osteoarthritis of the knee (or hip): The injection is intra-articular.
- Osteoligament or tendon lesions: injection of PRP directly on the injured area;
the injection is sometimes done under ultrasound control if the lesion is deep, allowing direct injection of the product into the lesion;
- after approximately 10 minutes of rest, the patient returns home.
PRP therapy is considered a state-of-the-art technique, and has been used for some years in Europe and the USA.
The preparation of PRP requires a blood sample, which is centrifuged to separate the platelets from the other blood elements (red and white blood cells). The cell separator allows in 15 minutes to increase the concentration of platelets and growth factors by more than 500%. The concentrated platelets are then re-injected into the pathological area. These platelets release growth factors in large numbers, up to eight times more, allowing the healing of damaged tissues, by stimulating local stem cells, and reducing inflammation and haemorrhage.
After the injection, it is advisable to avoid anti-inflammatories for 1 month, so as not to disturb the natural inflammatory reaction of PRP. But painkillers are allowed.
The number of injections varies according to the results, from 1 to 3 separated by 1 month. An inflammatory reaction with moderate pain is possible for 1 week.
